HA Pharmacology & Pharmacy – Unit 2
Drugs Acting on Autonomic Nervous System
CTEVT Second Year Health Science (PCL) | According to Syllabus 2024
Introduction to Autonomic Nervous System (ANS)
The Autonomic Nervous System regulates involuntary bodily functions through two main divisions: Sympathetic (SNS) “fight or flight” and Parasympathetic (PNS) “rest and digest”. Drugs acting on ANS either mimic or block neurotransmitters (acetylcholine, norepinephrine) at their receptors, allowing precise control of heart rate, blood pressure, bronchial tone, gastrointestinal motility, and glandular secretions.
1. Pharmacological Action of Acetylcholine (ACh)
Definition & Role
Acetylcholine is the primary neurotransmitter of:
- Parasympathetic nervous system (PNS)
- Somatic motor neurons (neuromuscular junction)
- Autonomic ganglia (both SNS & PNS)
- Central nervous system (CNS)
Metabolism: Rapidly hydrolyzed by acetylcholinesterase (AChE) at synapses.
Organ System Effects
- Heart: ↓ Heart rate (negative chronotropic), ↓ Force of contraction (negative inotropic)
- Smooth Muscle: Contraction (GI, bronchial, bladder)
- Glands: ↑ Secretion (salivary, sweat, lacrimal, gastric)
- Eye: Miosis (pupil constriction), accommodation for near vision
- CNS: Learning, memory, arousal (affected in Alzheimer’s)
📌 Clinical Applications:
- Diagnosis: Edrophonium test for myasthenia gravis (temporary improvement)
- Surgery: Acetylcholine used in ophthalmic surgery to induce miosis
- Therapeutic Limitation: Not used systemically due to rapid degradation and diffuse effects
2. Autonomic Receptors
Cholinergic Receptors
Muscarinic Receptors (M1-M5)
G-protein coupled receptors activated by ACh and muscarine
- M1: CNS, gastric parietal cells (↑ acid secretion)
- M2: Heart (↓ HR, ↓ AV conduction, ↓ contractility)
- M3: Smooth muscle (contraction), glands (secretion), endothelium (NO release → vasodilation)
- M4 & M5: Primarily in CNS (modulation)
Nicotinic Receptors (NN & NM)
Ligand-gated ion channels activated by ACh and nicotine
- NN (Neuronal): Autonomic ganglia (both SNS & PNS), adrenal medulla
- NM (Muscle): Neuromuscular junction (skeletal muscle contraction)
Adrenergic Receptors (Respond to Epinephrine/Norepinephrine)
| Receptor Type | Primary Locations | Major Actions | Clinical Drug Examples |
|---|---|---|---|
| Alpha-1 (α1) | Vascular smooth muscle, eye radial muscle, bladder sphincter, prostate | Vasoconstriction (↑BP), mydriasis, urinary retention | Phenylephrine (agonist), Prazosin (antagonist) |
| Alpha-2 (α2) | Presynaptic nerve terminals, CNS, platelets | Inhibits NE release (↓BP), sedation, platelet aggregation | Clonidine (agonist), Yohimbine (antagonist) |
| Beta-1 (β1) | Heart, kidney JG cells | ↑HR, ↑contractility, ↑AV conduction, renin release | Dobutamine (agonist), Metoprolol (antagonist) |
| Beta-2 (β2) | Bronchial smooth muscle, uterine muscle, liver, skeletal muscle vessels | Bronchodilation, uterine relaxation, glycogenolysis, vasodilation | Salbutamol (agonist), Propranolol (antagonist) |
α1 = Arteries, α2 = Auto-inhibit, β1 = Beats (heart), β2 = Breathing (lungs)
3. ANS Drug Classes: Comparison & Applications
Autonomic Nervous System Drug Classification
PARASYMPATHETIC
Stimulate PNS
Block PNS
SYMPATHETIC
Stimulate SNS
Block SNS
A. Parasympathomimetics (Cholinergic Agonists)
Direct-acting (Muscarinic Agonists)
Examples: Pilocarpine, Bethanechol, Carbachol
Mechanism: Directly bind & activate muscarinic receptors
Key Uses:
- Glaucoma (↓ intraocular pressure)
- Xerostomia (↑ salivary secretion)
- Post-operative ileus (↑ GI motility)
- Neurogenic bladder (↑ bladder contraction)
Indirect-acting (AChE Inhibitors)
Examples: Neostigmine, Pyridostigmine, Physostigmine, Edrophonium
Mechanism: Inhibit acetylcholinesterase → ↑ ACh levels
Key Uses:
- Myasthenia gravis (improves muscle strength)
- Alzheimer’s disease (cognitive symptoms)
- Reversal of neuromuscular blockade
- Glaucoma (chronic)
Side Effects & Contraindications
Side Effects (SLUDGE syndrome):
- Salivation, Lacrimation
- Urination, Diarrhea
- GI cramps, Emesis
- Bronchoconstriction, Bradycardia
Contraindications: Asthma, COPD, peptic ulcer, bradycardia, hypotension
B. Parasympatholytics (Anticholinergics)
Major Drugs & Uses
- Atropine: Bradycardia, pre-anesthetic, organophosphate poisoning
- Ipratropium/Tiotropium: Asthma/COPD (bronchodilation)
- Hyoscine (Scopolamine): Motion sickness, pre-op sedation
- Oxybutynin, Tolterodine: Overactive bladder (↓ urgency)
- Pralidoxime: Cholinesterase reactivator (OP poisoning)
Pharmacological Actions
- ↑ Heart rate (blocks M2)
- ↓ Glandular secretions (dry mouth, dry eyes)
- Bronchodilation (relaxes smooth muscle)
- ↓ GI motility & secretion
- Mydriasis & cycloplegia (eye)
- Urinary retention (relaxes bladder)
Adverse Effects & Contraindications
Side Effects (Dry as a bone, blind as a bat, red as a beet, mad as a hatter):
- Dry mouth, blurred vision
- Urinary retention, constipation
- Tachycardia, palpitations
- Confusion, hallucinations (elderly)
Contraindications: Glaucoma (angle-closure), BPH, GI obstruction, myasthenia gravis
D. Sympatholytics (Adrenergic Antagonists)
Alpha Blockers (α-antagonists)
Non-selective (α1+α2): Phentolamine, Phenoxybenzamine
α1 selective: Prazosin, Terazosin, Tamsulosin
Uses:
- Hypertension (α1 blockers)
- Pheochromocytoma (pre-op)
- BPH (improves urinary flow)
- Raynaud’s phenomenon
Side Effects: First-dose syncope, orthostatic hypotension, nasal congestion, reflex tachycardia
Beta Blockers (β-antagonists)
Non-selective (β1+β2): Propranolol, Nadolol, Timolol
β1 selective (cardioselective): Atenolol, Metoprolol, Bisoprolol
Uses:
- Hypertension, angina, MI
- Arrhythmias (supraventricular)
- Heart failure (selected β-blockers)
- Glaucoma (timolol eye drops)
- Migraine prophylaxis, anxiety
Side Effects: Bradycardia, fatigue, bronchospasm (non-selective), masking hypoglycemia, erectile dysfunction
Contraindications & Withdrawal
Beta Blocker Contraindications:
- Asthma/COPD (non-selective)
- Severe bradycardia/AV block
- Decompensated heart failure
- Peripheral vascular disease
Abrupt Withdrawal: Can cause rebound hypertension, tachycardia, angina exacerbation (taper slowly over 1-2 weeks)
One Page Summary: ANS Drugs
• Neurotransmitter of PNS, ganglia, NMJ
• Effects: ↓HR, ↑secretions, ↑GI motility, miosis
• Rapidly degraded by AChERECEPTORS
• Muscarinic (M1-M5): G-protein, PNS effects
• Nicotinic (NN, NM): Ion channels, ganglia & NMJ
• Adrenergic: α1 (vasoconstrict), α2 (inhibit), β1 (heart), β2 (lungs)PARASYMPATHOMIMETICS
• Direct: Pilocarpine (glaucoma, dry mouth)
• Indirect: Neostigmine (myasthenia gravis)
• SE: SLUDGE syndrome
• Contra: Asthma, bradycardiaSYMPATHOMIMETICS
• α1: Phenylephrine (decongestant, hypotension)
• β1: Dobutamine (cardiogenic shock)
• β2: Salbutamol (asthma)
• Mixed: Adrenaline (anaphylaxis, cardiac arrest)
• Atropine: Bradycardia, pre-anesthetic, OP poisoning
• Ipratropium: Asthma/COPD
• Oxybutynin: Overactive bladder
• SE: Dry mouth, blurred vision, urinary retention, tachycardia
• Contra: Glaucoma, BPH, GI obstructionSYMPATHOLYTICS
• α-blockers: Prazosin (HTN, BPH), SE: first-dose syncope
• β-blockers: Propranolol (non-selective), Metoprolol (β1 selective)
• Uses: HTN, angina, arrhythmias, migraine
• SE: Bradycardia, fatigue, bronchospasm
• Contra: Asthma, severe bradycardia, heart failureMNEMONICS
• SLUDGE: Salivation, Lacrimation, Urination, Diarrhea, GI cramps, Emesis
• α1 = Arteries, β1 = Beats, β2 = Breathing
• Anticholinergic: “Dry as a bone, blind as a bat, red as a beet, mad as a hatter”
Atropine for bradycardia, Adrenaline for anaphylaxis, Salbutamol for asthma, Pilocarpine for glaucoma
Clinical Application Scenarios
Scenario 1: Myasthenia Gravis
Presentation: Ptosis, diplopia, muscle weakness worsening through day.
Drug Choice: Pyridostigmine (AChE inhibitor)
Mechanism: ↑ ACh at NMJ → improves muscle strength
Monitoring: Muscle strength, respiratory function, cholinergic crisis vs myasthenic crisis
Scenario 2: Anaphylactic Shock
Presentation: Hypotension, bronchospasm, urticaria after bee sting.
Drug Choice: Adrenaline (Epinephrine) IM
Mechanism: α1 → vasoconstriction (↑BP), β2 → bronchodilation, β1 → cardiac support
Key: First-line, life-saving; administer immediately.
Scenario 3: Organophosphate Poisoning
Presentation: SLUDGE + muscle fasciculations, confusion, respiratory distress.
Drug Choice: Atropine + Pralidoxime
Mechanism: Atropine blocks muscarinic effects; Pralidoxime reactivates AChE
Priority: Airway management, atropine until secretions dry.
Visual Aid: ANS Receptor Actions
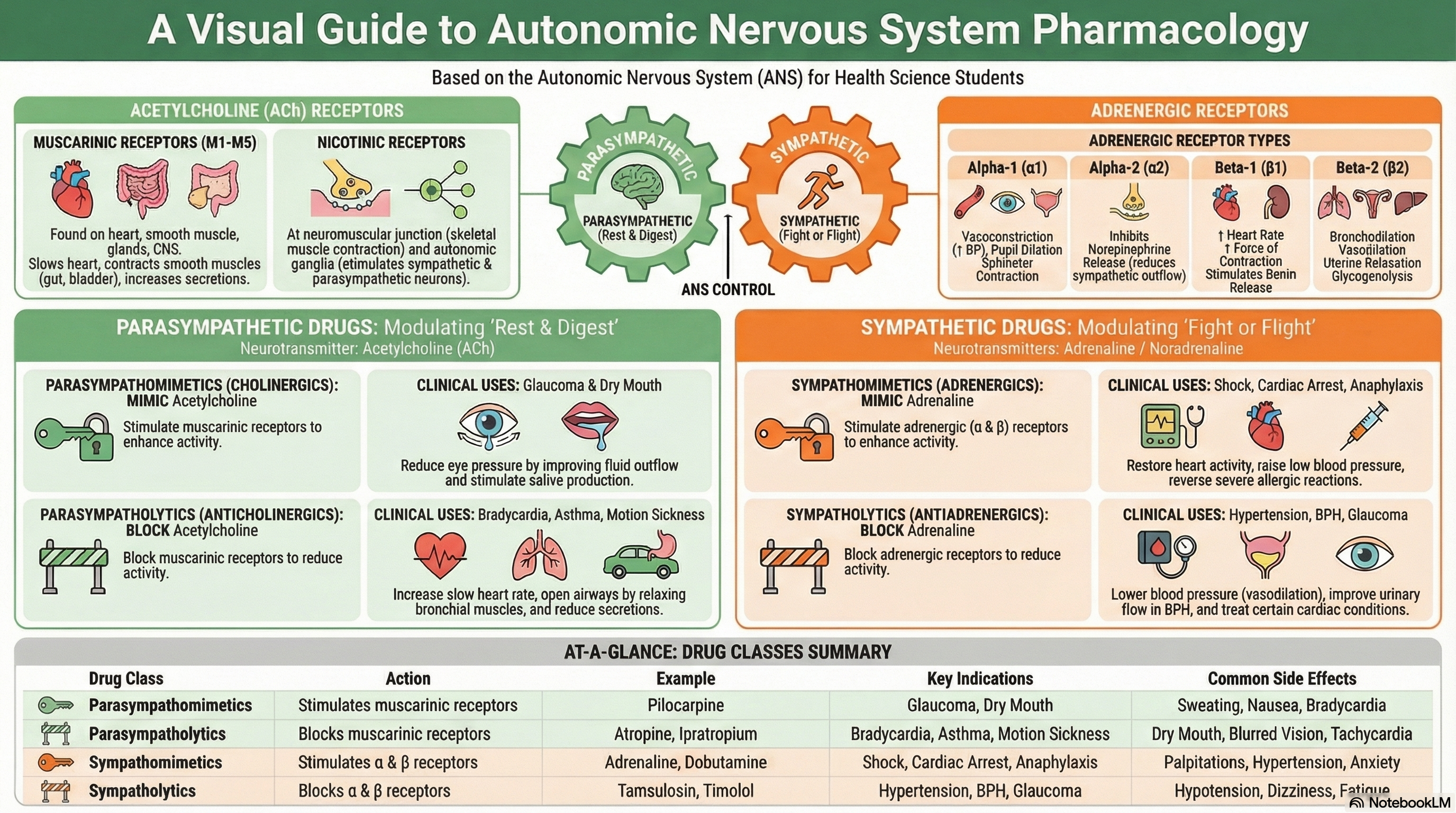
Topic Tags
Acetylcholine
Adrenergic Receptors
Parasympathomimetics
Parasympatholytics
Sympathomimetics
Sympatholytics
Atropine
Adrenaline
Beta Blockers
Alpha Blockers
Myasthenia Gravis
Glaucoma
Asthma
Anaphylaxis
Organophosphate Poisoning
CTEVT Syllabus
Health Assistant
HA Second Year
Pharmacology Notes
Key Clinical Takeaways
- ANS drugs work by mimicking or blocking neurotransmitters (ACh, NE/E) at specific receptors.
- Parasympathomimetics cause SLUDGE; Parasympatholytics cause dry mouth, blurred vision, tachycardia.
- Adrenaline is first-line for anaphylaxis (α1, β1, β2 effects).
- Beta-blockers must be tapered to avoid rebound hypertension/angina.
- Atropine is antidote for organophosphate poisoning and bradycardia.
- Receptor selectivity determines drug’s therapeutic use and side effect profile.
Quick Self-Check
Question 1: Which drug class would you choose for acute bronchospasm in asthma?
Question 2: Match the drug to its primary use:
Download Notes
Get a printable PDF version of these comprehensive ANS pharmacology notes. HA Pharmacology and Pharmacy Unit 2 Drugs Acting on Autonomic Nervous System Notes
Includes all drug classes, receptors, clinical uses, and one-page summary. HA Pharmacology and Pharmacy Unit 2 Drugs Acting on Autonomic Nervous System Notes
Further Reading & Resources
- Official CTEVT Syllabus: CTEVT Website
- American Heart Association Guidelines: AHA Guidelines (for adrenaline in cardiac arrest)
- Global Initiative for Asthma (GINA): GINA Guidelines (for bronchodilators)


