HA Pharmacology & Pharmacy – Unit 1
General Pharmacology – CTEVT Second Year Notes
According to CTEVT Syllabus (2024) | Health Science (PCL)
Introduction to Pharmacology
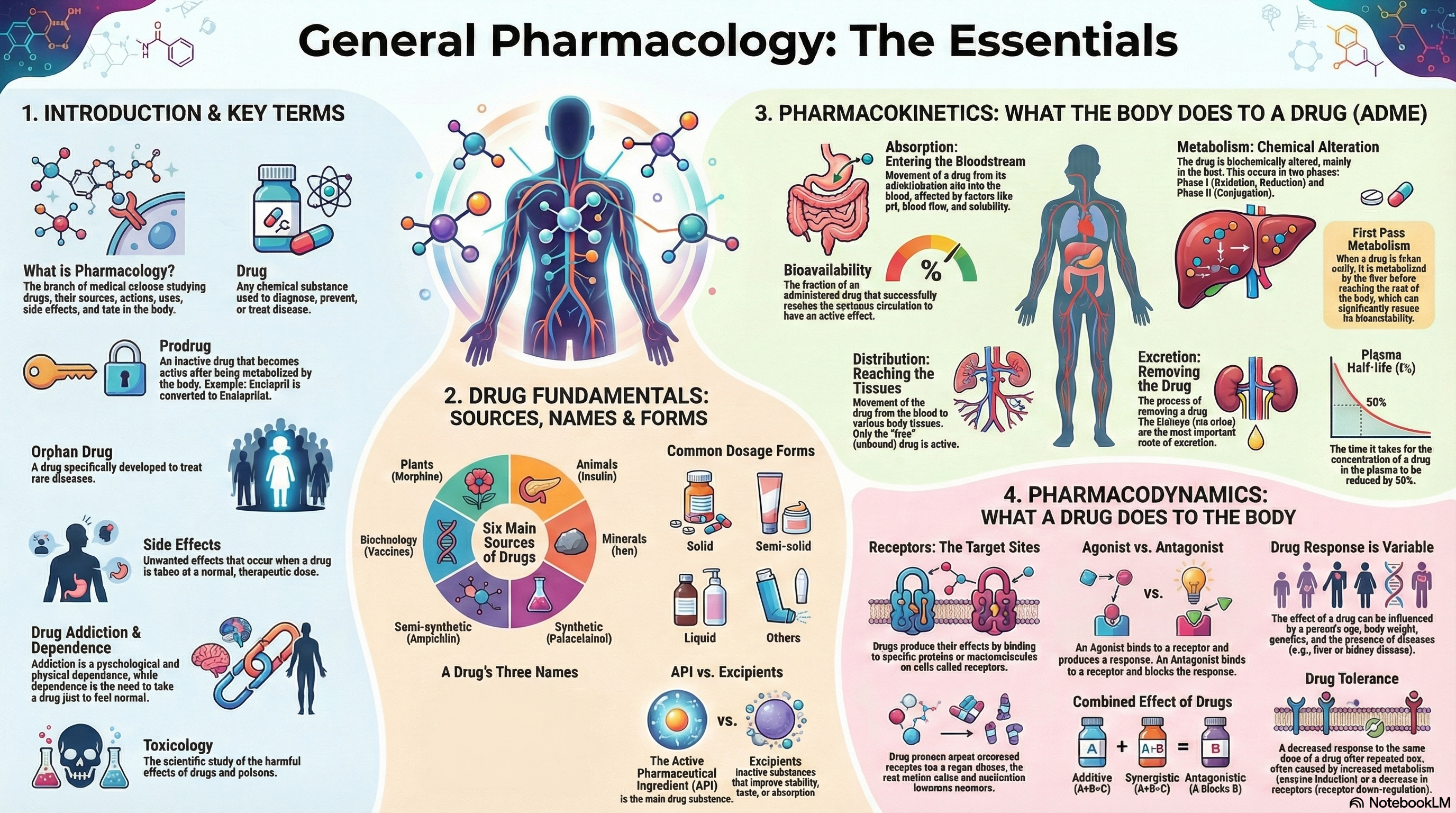
Pharmacology is the scientific study of drugs—their sources, properties, effects, and interactions with living systems. This unit forms the foundation for understanding how medications work, how they’re administered, and how the body processes them. Mastery of these principles is essential for safe and effective clinical practice.
1. Important Terms in Pharmacology
DrugAny chemical substance used to diagnose, prevent, or treat disease.
MedicineA drug prepared in a suitable dosage form for patient administration.
ProdrugInactive drug that becomes active after metabolism (e.g., Enalapril → Enalaprilat).
Orphan DrugDrug developed specifically to treat rare medical conditions.
Side EffectsUnintended, usually mild effects occurring at normal therapeutic doses.
ToxicologyStudy of harmful effects of drugs, chemicals, and poisons on living systems.
2. Sources of Drugs
- Plant Source: Morphine (opium poppy), Atropine (belladonna), Digoxin (foxglove)
- Animal Source: Insulin (pancreas), Heparin (intestine/lung), Vaccines
- Mineral Source: Iron sulfate, Magnesium sulfate (Epsom salt), Aluminum hydroxide
- Synthetic: Paracetamol, Aspirin, Sulfonamides
- Semi-synthetic: Ampicillin (from penicillin), Steroids
- Biotechnology: Human insulin, Monoclonal antibodies, Recombinant vaccines
3. Drug Nomenclature
Example: Paracetamol
- Chemical Name: N-acetyl-para-aminophenol
- Generic Name: Paracetamol (Acetaminophen)
- Brand Name: Crocin, Tylenol, Panadol
Exam Tip: Generic names are most important for exams and prescriptions as they’re universal.
4. Dosage Forms & Routes of Administration
Classification of Dosage Forms
Solid Forms
- Tablets (scored, coated)
- Capsules (hard/soft)
- Powders (bulk/divided)
Semi-solid
- Ointments (greasy)
- Creams (water-based)
- Gels (transparent)
Special Forms
- Suppositories (rectal)
- Pessaries (vaginal)
- Inhalers (aerosols)
Routes of Drug Administration
| Route | Advantages | Disadvantages | Examples |
|---|---|---|---|
| Oral | Safe, convenient, economical | First-pass metabolism, slow onset | Tablets, capsules, syrups |
| Intravenous (IV) | Rapid action, 100% bioavailability | Risk of infection, anaphylaxis | Emergency drugs, antibiotics |
| Intramuscular (IM) | Faster than oral, depot preparations | Painful, tissue damage risk | Vaccines, analgesics |
| Subcutaneous (SC) | Slow, sustained absorption | Not for large volumes | Insulin, heparin |
| Topical | Local effect, minimal systemic absorption | Limited to superficial conditions | Ointments, creams, lotions |
5. Dose Concepts
Loading Dose
Higher initial dose to achieve therapeutic concentration quickly.
Example: Digoxin for rapid atrial fibrillation control.
Maintenance Dose
Lower subsequent doses to maintain steady therapeutic effect.
Example: Daily antibiotics after initial loading.
Fixed Dose Combination (FDC)
Two or more drugs in single preparation.
Example: Amoxicillin + Clavulanic acid (Augmentin).
6. Pharmacokinetics (ADME)
ADME Concept
Absorption
Distribution
Metabolism
Excretion
Mnemonic: A Dog Must Eat (Absorption, Distribution, Metabolism, Excretion)
Absorption
Definition: Movement from site of administration to bloodstream.
Key Factors:
- Drug solubility (lipid vs water soluble)
- pH and ionization state
- Blood flow at absorption site
- First-pass metabolism (oral route)
Distribution
Definition: Reversible transfer of drug between blood and tissues.
Key Concepts:
- Volume of Distribution (Vd): Theoretical volume needed to contain total drug at plasma concentration
- Plasma Protein Binding: Drugs bind to albumin (acidic drugs) and α1-acid glycoprotein (basic drugs)
- Only free (unbound) drug is active
Barriers: Blood-brain barrier, placental barrier
Metabolism
Primary Site: Liver (hepatic microsomal enzymes)
Phases:
- Phase I: Oxidation (CYP450), Reduction, Hydrolysis
- Phase II: Conjugation (Glucuronidation, Sulfation)
Excretion
Primary Route: Kidney (glomerular f
glomerular filtration, tubular secretion)
Other Routes: Bile (enterohepatic circulation), Lungs, Sweat, Breast milk
Key Parameters:
- Half-life (t½): Time for plasma concentration to reduce by 50%
- Clearance: Volume of plasma cleared of drug per unit time
Dosing Interval: Usually every 1-2 half-lives
7. Pharmacodynamics
Key Concept
“What the body does to the drug”
ADME Processes
“What the drug does to the body”
Effects & Mechanisms
Drug-Receptor Interactions
Affinity: Ability to bind to receptor
Intrinsic Activity: Ability to produce effect after binding
High affinity + High activity
High affinity + No activity
Receptor Types: GPCRs (most common), Ion channels, Enzyme-linked, Nuclear receptors
Combined Drug Effects
Drug Tolerance & Factors
Tolerance: Decreased response with repeated use
Mechanisms:
- Enzyme induction (faster metabolism)
- Receptor down-regulation
- Pharmacodynamic adaptation
Influencing Factors:
- Age (neonates, elderly)
- Body weight/composition
- Genetic variations (pharmacogenomics)
- Liver/kidney function
One Page Summary
• Drug: Diagnostic/therapeutic chemical
• Prodrug: Activated in body
• Orphan drug: Rare diseases
• Side effect: Unwanted at normal dose
• Tolerance: Decreased responseSOURCES
• Plant: Morphine, Digoxin
• Animal: Insulin, Heparin
• Synthetic: Paracetamol
• Biotechnology: Vaccines, mAbsNAMES
• Chemical: Structure-based
• Generic: Official name
• Brand: Company nameDOSAGE FORMS
• Solid: Tablets, capsules
• Liquid: Syrups, suspensions
• Semi-solid: Ointments, creams
• Special: Suppositories, inhalers
• Oral: Safe, slow, first-pass
• IV: Fast, 100% bioavailability
• IM: Moderate speed, painful
• SC: Slow, sustained (insulin)
• Topical: Local effectPHARMACOKINETICS (ADME)
• Absorption: To bloodstream
• Distribution: Blood to tissues
• Metabolism: Liver (Phase I/II)
• Excretion: Kidney (main)
• Half-life: Time for 50% decreasePHARMACODYNAMICS
• Agonist: Produces effect
• Antagonist: Blocks effect
• Additive: 1+1=2 effect
• Synergism: 1+1>2 effect
• Tolerance: Reduced response
Topic Tags
Drug SourcesDosage Forms
Routes of Administration
Pharmacokinetics
Pharmacodynamics
ADME
Bioavailability
Half-life
First-pass Metabolism
Agonist Antagonist
Drug ToleranceCTEVT Syllabus
Health Assistant
Fixed Dose Combination
Prodrug
Orphan Drug
Volume of Distribution
Plasma Protein Binding
HA Second Year
Key Takeaways
- Pharmacokinetics (ADME) describes drug movement in the body; Pharmacodynamics describes drug effects on the body.
- Route selection depends on drug properties, desired onset, and patient condition.
- Only free (unbound) drug is pharmacologically active; protein-bound drug serves as reservoir.
- First-pass metabolism significantly reduces oral bioavailability of many drugs.
- Understanding tolerance mechanisms helps prevent therapeutic failure and dependence.
- Generic names are essential for safe prescribing and avoiding medication errors.
Quick Self-Check
Question: Which route bypasses first-pass metabolism completely?
Further Reading & Resources
- Official CTEVT Syllabus: CTEVT Website
- WHO Essential Medicines List: WHO EML
- Pharmacology Education Resources: Pharmacology Education