PHARMACOLOGY & PHARMACY
Unit 3: Drugs Acting on Peripheral Nervous System
CTEVT Health Science Second Year | Syllabus 2024
🧠 Introduction to PNS Drugs
Drugs acting on the Peripheral Nervous System (PNS) target nerves outside the brain and spinal cord. This unit focuses on two key classes: Skeletal Muscle Relaxants (which reduce muscle tone and spasm) and Local Anesthetics (which block pain signals in specific areas). Understanding their mechanisms, uses, and adverse effects is crucial for safe clinical practice.
💊 Skeletal Muscle Relaxant Drugs
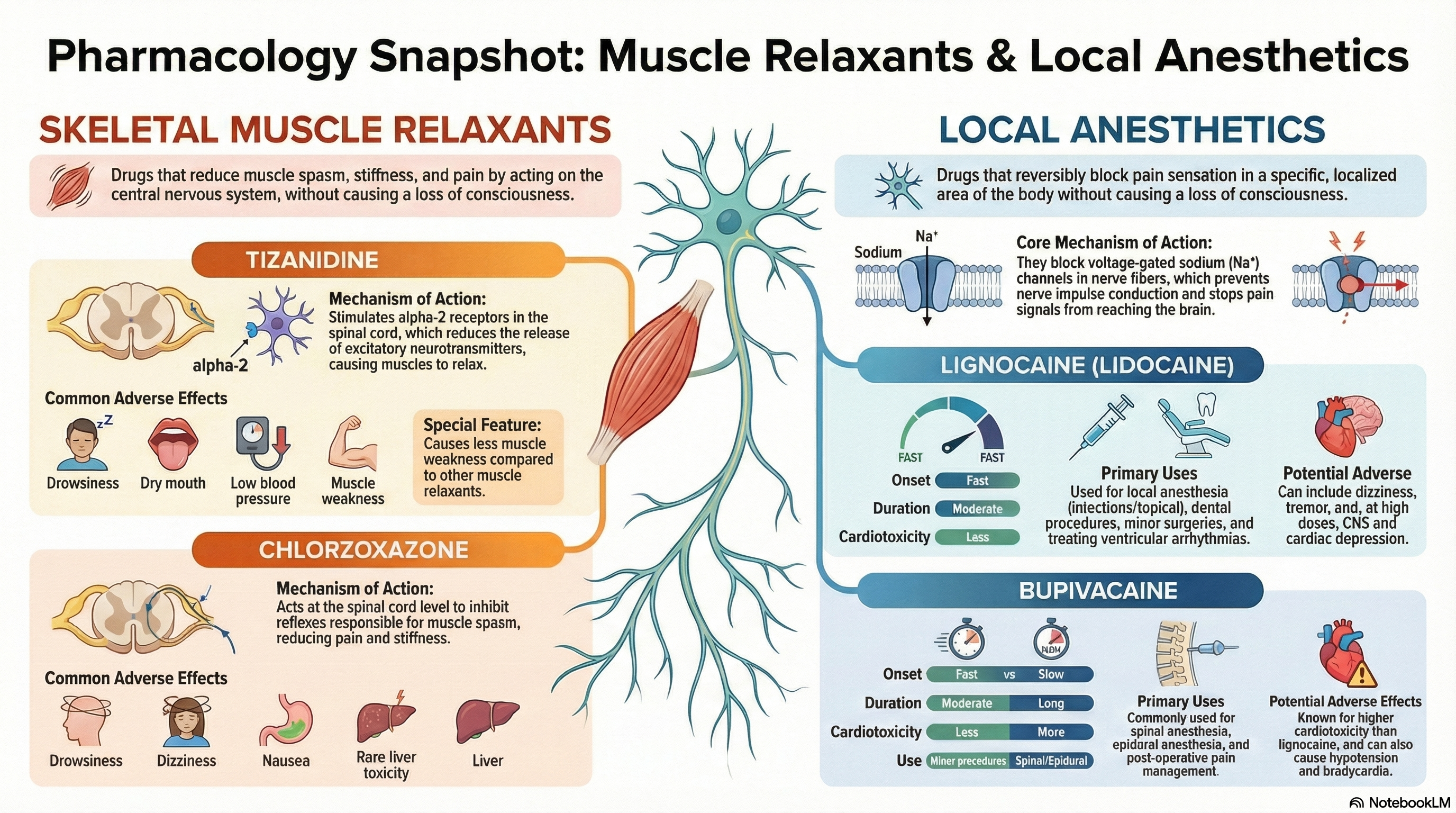
Definition: Drugs that reduce muscle spasm, stiffness, and pain without causing loss of consciousness. They primarily act centrally (on the CNS).
Tizanidine
⚙️ Mechanism of Action
Stimulates alpha-2 receptors in spinal cord → decreases release of excitatory neurotransmitters (e.g., glutamate) → reduces muscle tone and spasm.
✅ Uses
- Muscle spasm (acute/chronic)
- Spasticity due to stroke, MS, spinal injury
- Multiple sclerosis-related spasticity
⚠️ Adverse Effects
Dry mouth
Hypotension
Muscle weakness
Chlorzoxazone
⚙️ Mechanism of Action
Acts at spinal cord level → inhibits polysynaptic reflexes responsible for muscle spasm → reduces pain and stiffness.
✅ Uses
- Acute musculoskeletal pain
- Muscle spasm (short-term relief)
- Painful conditions (e.g., back pain)
⚠️ Adverse Effects
Dizziness
Nausea
Liver toxicity
📊 Comparison: Tizanidine vs Chlorzoxazone
| Feature | Tizanidine | Chlorzoxazone |
|---|---|---|
| Class | α₂-agonist | Central muscle relaxant |
| Primary Use | Spasticity (chronic) | Acute muscle spasm |
| Key Side Effect | Hypotension | Hepatotoxicity (rare) |
| Duration of Therapy | Long-term possible | Short-term only |
🩺 Local Anesthetics
Definition: Drugs that reversibly block pain sensation in a localized area without loss of consciousness.
🔬 Mechanism of Action (CRITICAL)
Block voltage-gated sodium (Na⁺) channels in nerve fibers → prevent depolarization → nerve impulse conduction stops → pain signals do not reach the brain.
Lignocaine (Lidocaine)
✅ Uses
Dental procedures
Minor surgery
Ventricular arrhythmias
⚠️ Adverse Effects
- CNS: Dizziness, tremor, seizures (high dose)
- Cardiac: Depression, bradycardia
- Allergic reactions (rare)
Bupivacaine
✅ Uses
Epidural anesthesia
Nerve blocks
Post-op pain
⚠️ Adverse Effects
- Cardiotoxicity (ventricular arrhythmias)
- Hypotension
- Bradycardia
- CNS toxicity at high doses
📊 Comparison: Lignocaine vs Bupivacaine
| Parameter | Lignocaine | Bupivacaine |
|---|---|---|
| Onset | Rapid (2-5 min) | Slow (10-20 min) |
| Duration | Moderate (1-2 hr) | Long (4-8 hr) |
| Potency | Moderate | High (4x lignocaine) |
| Toxicity | CNS > Cardiac | Cardiac > CNS |
| Key Use | Infiltration, dental, arrhythmias | Spinal/epidural, prolonged pain relief |
🧠 Memory Aids & Mnemonics
Local Anesthetic Onset
“Lidocaine is Lightning, Bupivacaine is a Breeze”
Lidocaine = Fast onset (Lightning), Bupivacaine = Slow onset (gentle breeze)
Tizanidine Mechanism
“Alpha-2, Relaxes You”
Stimulates alpha-2 receptors → muscle relaxation
Local Anesthetic Toxicity
“Bupivacaine Bothers the Heart”
Bupivacaine has higher cardiotoxicity than lignocaine
📄 ONE PAGE SUMMARY
Skeletal Muscle Relaxants
- Tizanidine: α₂-agonist, for spasticity, causes hypotension
- Chlorzoxazone: Central acting, for acute spasm, hepatotoxicity risk
Local Anesthetics
- Mechanism: Block Na⁺ channels
- Lignocaine: Fast, moderate duration, for infiltration
- Bupivacaine: Slow, long duration, cardiotoxic
Key Differences
- Tizanidine: α₂-agonist vs Chlorzoxazone: central
- Lignocaine: fast vs Bupivacaine: slow onset
- Bupivacaine: more cardiotoxic
Download Complete Notes
Get a printable PDF with all drug tables, mechanisms, and exam tips. HA Pharmacology and Pharmacy Unit 3 Drugs Acting on Peripheral Nervous System Notes
![]()
![]()
🏷️ Related Topics
Local Anesthetics
Tizanidine
Chlorzoxazone
Lignocaine
Bupivacaine
Pharmacology CTEVT
Na+ Channel Blockers
Muscle Spasm Drugs
Anesthesia Pharmacology
Peripheral Nervous System
Alpha-2 Agonists
Amide Anesthetics
Spasticity Treatment
Nerve Block Drugs
Drug Mechanisms
Adverse Effects
CTEVT Syllabus 2024
Health Science Notes
Medical Pharmacology
© CTEVT Health Science Second Year | Pharmacology Unit 3 Notes – HA Pharmacology and Pharmacy Unit 3 Drugs Acting on Peripheral Nervous System Notes
Source: CTEVT Syllabus 2024 | For academic use only


